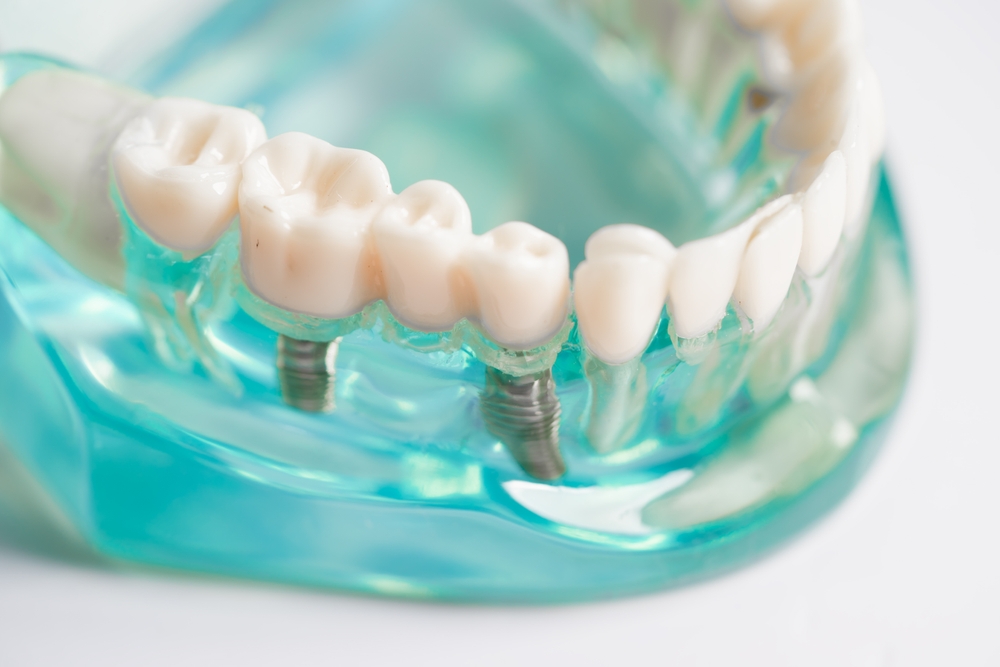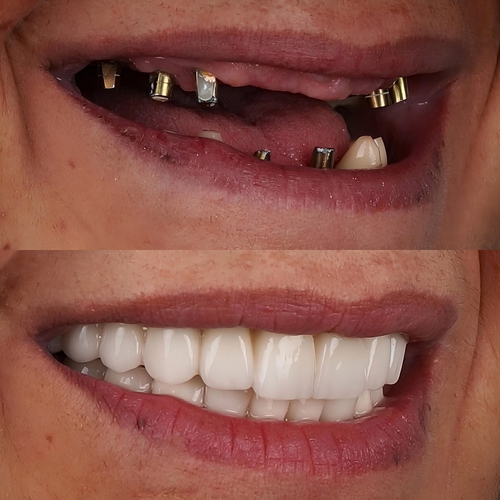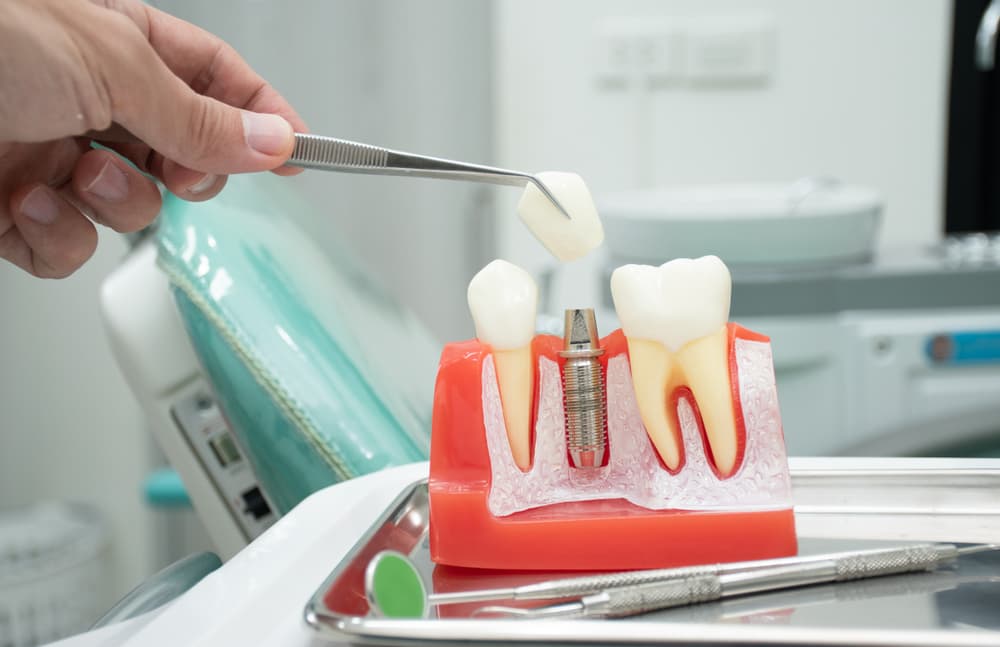
Losing teeth is a significant change that affects much more than just your smile. Your jawbone needs the steady pressure of chewing to remain strong and retain its original shape. Without that stimulation, the bone shrinks over time. This can affect your bite, the way dentures fit, and even your overall facial appearance.
High-quality All-on-4 implants in San Marcos, CA, are designed to replace a full arch of teeth using four carefully placed dental implants to create a secure foundation that feels far more natural than traditional dentures. While most people think of implants in terms of improved confidence and comfort in everyday situations, they play a key role in preserving oral health, and specifically protect the jawbone density and shape.
In today’s article, we look at why bone loss tends to follow tooth loss and explore the benefits of all-on-4 dental implants for jawbone preservation to illustrate why All-on-4 is a superior solution for healthier bone and oral wellbeing than traditional dentures.
Can missing teeth cause jaw problems?
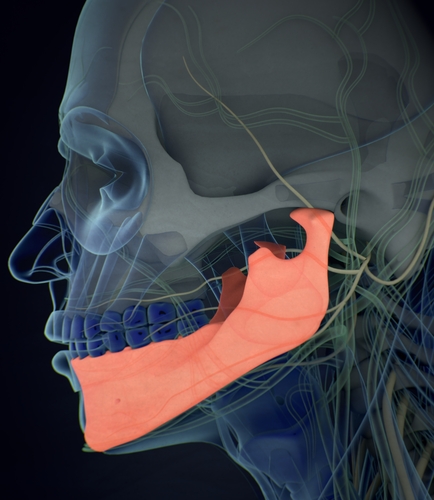
Once teeth are gone, that pressure and root-based stimulation disappear. Our body interprets this as a loss of function and starts breaking down the bone because it’s no longer needed.
If left untreated, the bone loss adds up and creates a domino effect. The ridge that used to hold the teeth becomes thinner, narrower, and shorter. This, in turn, causes changes to the gumline, and the lower part of your face starts looking ‘collapsed’ due to a lack of support.
In practical terms, less bone makes all future dental treatments more complicated because it gives your dentist less structure to work with.
The main point is this: you shouldn’t wait too long to replace missing teeth, or you risk serious jawbone issues and general oral health complications.
Do regular dentures cause bone loss?
Traditional dentures sit on top of gums and rely on suction, adhesives, and the dental ridge to stay in place. While they can improve appearance and help with eating and speaking, they don’t replace tooth roots. This means they can’t mimic your original teeth and deliver the kind of pressure and stimulation your jawbone needs to stay strong and healthy.
This is the main reason why people who wear dentures for a long time notice that the fit changes as the years go by. Dentures start feeling loose and uncomfortable, in some cases, slipping and requiring frequent relines. Many patients then find themselves in a vicious cycle: bone shrinks, dentures fit worsens, and adjustments become routine.
How do all-on-4 implants prevent jawbone loss?
Instead of placing an implant for every missing tooth, All-on-4 implants are strategically placed in key areas of the mandible to support a full set of fixed replacement teeth. The front pair of implants is usually placed more vertically, while the back pair is angled to maximize contact with the available bone for greater stability.
Because implants support a firmly fixed arch of replacement teeth, they don’t sit on gums like removable dentures do. This not only feels more like natural teeth and ensures a stable bite, but it also provides enough pressure and stimulation to the jawbone to preserve its structural integrity.
What are the key benefits of All-on-4 dental implants?
Placement, design, and function introduce numerous benefits of all-on-4 dental implants for jawbone preservation compared to traditional dentures. All-on-4 also avoids many of the issues associated with traditional dentures, like instability, sore spots, and lack of structural support for facial tissues.
1. Restores the stimulation your jawbone needs
If we compare all-on-4 vs dentures for maintaining jawbone density, one of the biggest benefits is biomechanical. Since implants are anchored directly in the bone, the pressure is transferred into the jaw when you chew. This mimics the normal function of natural teeth and keeps your bone active and supported.
While no treatment can guarantee ‘zero’ bone change over time, compared to removable dentures and leaving space where a tooth once was, implants significantly slow the rate of bone loss.
2. Helps preserve the alveolar ridge
After tooth loss, the alveolar ridge (the part of the jawbone that holds teeth) can shrink significantly. All-on-4 dental implants help stop bone resorption by providing anchored support that preserves ridge integrity and gives the bone something to ‘work around.’
Keeping the ridge healthier isn’t just about appearance. It also supports the gums better and contributes to increased bite stability over time.
3. Reduces constant pressure on gums & ridge
Since removable dentures rely on soft tissue and the alveolar ridge for support, it can lead to denture compression from dentures pressing too hard. With firmly fixed All-on-4’s, there is no danger of this. Since it’s attached to implants, it doesn’t press down on the gums during chewing.
The difference is less rubbing, fewer sore spots, less discomfort, and more ease in day-to-day situations, especially for people struggling with denture movement.
4. Provides better bite stability
When your dentures feel loose, it’s hard to enjoy care-free meals and chew normally. In those cases, people tend to compensate and avoid certain foods, chew on one side, or reduce their bite force. This is not only frustrating as it affects your diet and prevents you from enjoying your favorite foods, but it also leads to an uneven strain in the jaw, which brings us back to the problem of an unstimulated jawbone that leads to bone loss.
Built for stability, a strong bite, and more natural chewing patterns, All-on-4 dental implants help stop bone resorption. When chewing feels normal, it becomes more symmetrical and delivers consistent, healthy pressure to the bone.
5. Supports facial structure over time
Many people are surprised to learn just how much jawbone loss can change their facial appearance. As the bone shrinks, the lower face starts losing support. The distance between the nose and chin shortens and the lips lose support as the bone loses volume. While this is alarming, it’s not simply an aesthetic concern. It’s also a structural problem tied to jawbone density and overall health.
All-on-4 implants prevent jawbone loss by preserving the underlying support that keeps the face looking fuller and healthier. Restored bite height plays a role in avoiding the ‘sunken’ appearance that can happen to individuals wearing dentures.
6. Prevents the need for bone grafting
When tooth loss is left untreated, progressive bone loss can limit future implant placement options. Once their jawbone deteriorates beyond a certain point, patients may require bone grafting to rebuild volume before dental implants can be placed. All-on-4 is often placed strategically to maximize available bone density and eliminate the need for grafting.
That being said, timing matters, so it’s highly recommended that you contact our specialists as soon as tooth loss occurs. The sooner missing teeth are replaced with All-on-4 implants, the more bone you’ll be able to preserve.
Who should I call for reliable All-on-4 implants in San Marcos, CA?
If you’re not sure if you’re a good candidate for All-on-4, want to inquire about the serious risk of dental tourism, or have any questions about All-on-4 dental implants, we’ll gladly help you make sense of all this and so much more.
To elevate your day-to-day experience and indulge in your favorite meals with comfort and a care-free smile, book your appointment today!

 1. Dental implant procedure is not a one-time appointment
1. Dental implant procedure is not a one-time appointment Visiting Mexico, Costa Rica, or Colombia is a great choice for a memorable holiday, but for dental treatments, on the other hand, less so. The best way to ensure long-term comfort, functionality, and appearance of your dental implants is to visit the Temecula Center for Dental Implants.
Visiting Mexico, Costa Rica, or Colombia is a great choice for a memorable holiday, but for dental treatments, on the other hand, less so. The best way to ensure long-term comfort, functionality, and appearance of your dental implants is to visit the Temecula Center for Dental Implants. 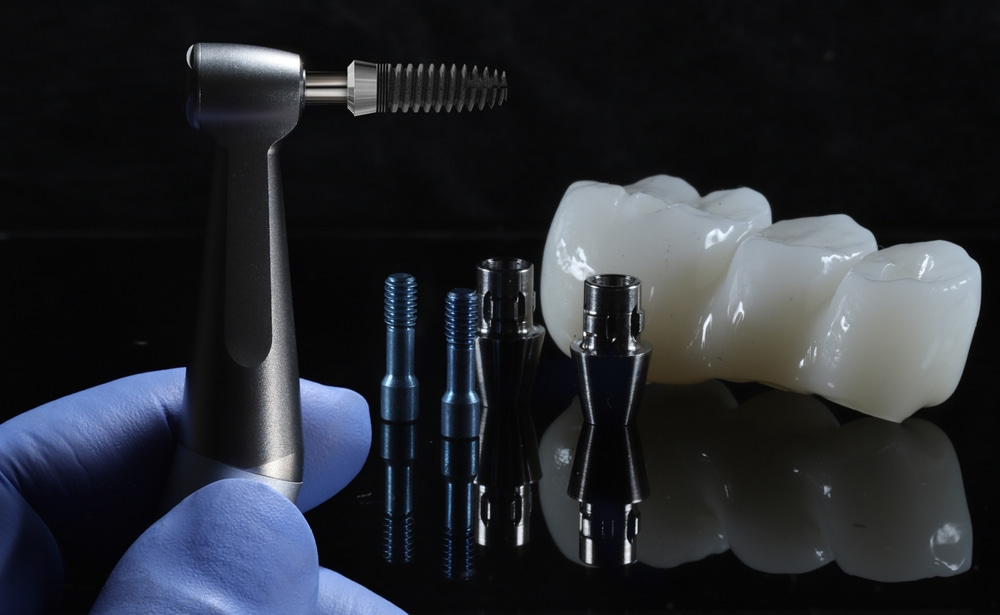
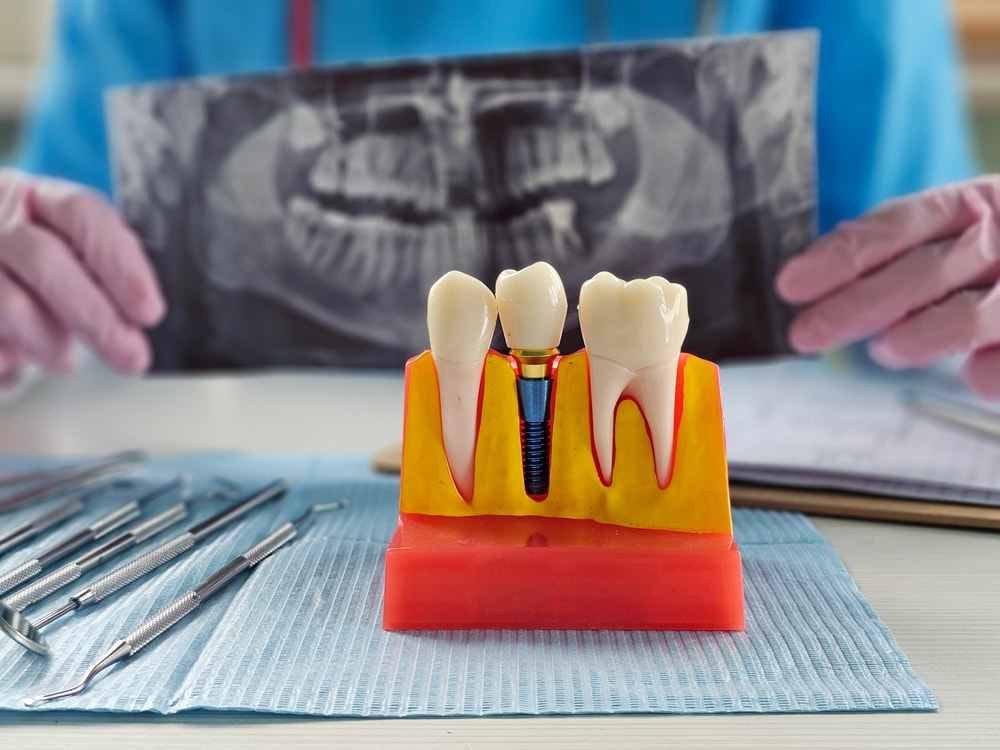






 If you’re looking to make a smart investment in your long-term oral health, appearance, and confidence, Temecula Center for Dental Implants is the leading clinic in
If you’re looking to make a smart investment in your long-term oral health, appearance, and confidence, Temecula Center for Dental Implants is the leading clinic in